
Abuja, Nigeria Aisha Aliyu is eight-months pregnant and sprawled out on a mat in front of her house with four of her children spread around her feet. Two-year-old Hauwa and five-year-old Abba are both crying and tugging at their mother’s coffee-colored hijab. She, in response, rolls her eyes and clicks her tongue at them. She looks tired.
The child Aliyu is carrying is her tenth. The last four were delivered in the Durumi Camp, a place in Nigeria’s capital city, Abuja, that she and an estimated more than 3,000 other internally displaced people call home.
In 2013, Aliyu fled her home in the village of Wala in Nigeria’s northeastern Borno State to its capital, Maiduguri. She said her village was attacked and much of it burned down by armed Islamist group, Boko Haram. Two years later, the militant group attacked Maiduguri, forcing Aliyu to again migrate, this time travelling over 856km south to Abuja with her husband and five children.
The now 39-year-old saw having many children as a way of replacing her relatives killed by the insurgents, but reveals she was done after her last pregnancy in 2021 and began using contraceptives. However, she became pregnant again this year.
Having already borne children in Durumi camp (one of 264 communities for internally dispaced people (IDPs) known to exist across Nigeria as of September 2021), Aliyu was fearful, knowing of the limited resources she would have access to. The farmer’s wife had been unable to afford the food and medication she needed to stay healthy, and antenatal services were limited.

Aisha with five of her children
The space initially set up as a birthing suite at the camp was rudimentary and barely hygienic, explains Liyatu Ayuba, appointed the camp ‘s Women’s Leader by the site’s Chairman when she arrived in 2014. She has since handled issues regarding health, food or children on behalf the IDPs.
“It was a tent that we swept, and I would put a mat or wrapper on the floor for the women to lie down on to give birth,” says Ayuba, who for much of the camp’s history has been its only birth attendant. Many of the displaced women refer to her as Mama.
Ayuba says the tent was a shanty built with corrugated roofing sheets and a sandy floor. If gloves were available, the birth attendant used them and if not, she explains that she covered her hands with polythene bags and cut umbilical cords with a razor blade.
“I gave birth to three of [my children] with Mama’s help on a mat under the shelter,” Aliyu reports, referring to the birthing tent. “Mama cut the umbilical cord and bathed the baby.”
In 2019, a non-governmental organization set up the camp’s health post where Aliyu’s ninth child, Hauwa, was delivered in 2021. The post is a small clinic located inside a repurposed 20ft shipping container, where wooden boards partition the space to create a delivery suite which looks more like a storage space and just about holds a bed, a baby cot, a drip stand, a broken chair, a trolley and empty containers that should contain water. The other half is the consultation room with a table, two chairs, a bed, and a cupboard where medicines and devices are kept.
Though basic, the clinic at least provides a consultation space that women previously had to make do without and Ayuba is proud to say the camp has not recorded any deaths among mothers or babies under her watch.

The makeshift delivery room partitioned in the shipping container used as the camp’s health post
‘No ‘special arrangement’ for those who are pregnant in Nigeria’s camps
Aliyu is one of many internally displaced women bearing children in Nigeria’s camps, with some grounds not even housing a health post or shelter for birth, instead needing women to go into labour in their own shelters or that of their birth attendant.
A 2021 PhD thesis by Fatima Mahmood Jibirilla at Walden University, states that women living in IDP camps in Nigeria “have a higher risk of maternal death than women living in their homes.” The author cited a range of factors increasing the risk of maternal and neonatal deaths in these settings, including inadequate prenatal care services and limited family planning programs.
“There are no special arrangements for pregnant women in IDP and refugee camps [in Nigeria]. There are poor antenatal services that are inadequate to detect and address likely pregnancy-related complications and other signs of poor pregnancy outcomes,” the author writes. While there have been no maternal or infant deaths at Durumi on her watch, according to Ayuba, multiple doctors volunteering there and across camps in Abuja corroborated the concerns highlighted in the study to FN.
In a country that has long had among the highest maternal mortality rates in the world and has the third highest number of internally displaced people (IDPs) in Africa as of the end of 2022, according to the Internal Displacement Monitoring Centre (IDMC), the lack of adequate maternal healthcare provision in these camps is a significant concern, one of the doctors told FN.
The 2022 IDMC figures also show that 4.5m Nigerians were classed as “internally displaced people” as a result of both conflict and natural disasters, with flooding outstripping protracted violence as the main source of displacement.
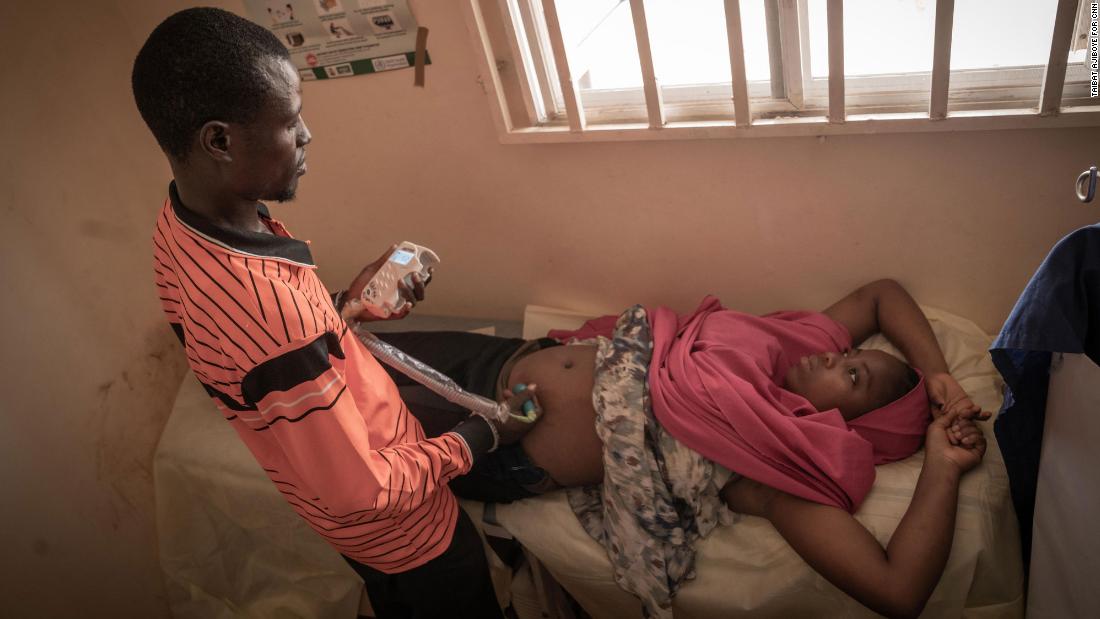
The camp nurse, Isa Umar examines a pregnant woman during antenatal session
While there is no national breakdown of IDPs by sex or age, a 2023 report by the Camp Coordination and Camp Management (CCCM) Sector says there are 1,575,741 women and children in the Nigerian states of Borno, Adamawa, and Yobe alone, making up 74% of the 2,124,053 IDPs in those states.
Nigeria’s total IDP population relies largely on the graces of charitable organizations for its health care, Ayuba and the camp’s nurse Isa Umar told FN.
‘If it happens, I am dead.’ The prohibitive costs of care
Wednesdays are antenatal day in Durumi. When FN visits, camp nurse Isa Umar, who himself was forced to leave his home due to the insurgency, is in the consultation room using a handheld ultrasound scanner to monitor a baby’s growth and a fetoscope to monitor the heartbeat among the expectant mothers coming in.
Umar measures each pregnant woman’s stomach followed by her weight. After they’ve been seen, women compare notes while sitting on the clinic’s veranda, discussing how any of the medicines Umar has prescribed will be paid for.
The set up is far from adequate. Umar tells FN: “We don’t even have folic acid or anti-malarial medicine to give them. I have to write these for them to go and buy.” Malaria is endemic in Nigeria and infections pose various risks during pregnancy, such as premature labour and miscarriage, and folic acid is recommended for those who are pregnant or planning to become pregnant, to reduce the risk of certain birth defects.
But for most of the 64 women recorded in the camp’s birth register this year, these costs are prohibitive. Folic acid, for example, costs ₦3,000 ($3.74) for 100 tablets and Aliyu tells FN she could not possibly have afforded that cost for the duration of her pregnancy. She says she’s only been able to take this vital supplement when NGOs have donated them free of charge. Back home in Wala, her N100 ($0.11) hospital card had entitled her to free folic acid as well as other resources while pregnant.
Getting clean water at the camp is also a challenge, Aliyu shares, explaining that it’s a time-consuming, strenuous task requiring her to make several trips daily and is one she can no longer do in the final weeks of her pregnancy. Instead, she now pays for it to be delivered. At its cheapest, enough water to make the family’s breakfast of pap (porridge made from ground corn) and other domestic chores for a month costs ₦24,000 ($28.43). Costs can rise by 25% on days when there is no electricity and a generator is needed to work the pumps, or when water sellers must go farther to fetch it.
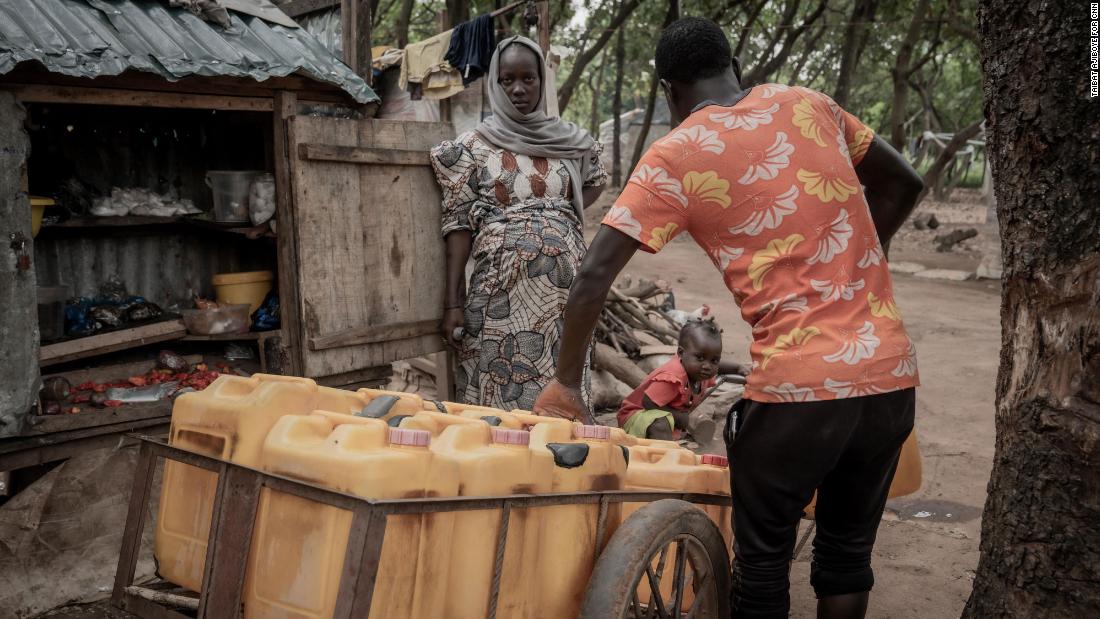
With Aisha almost full term, she is no longer able to go to fetch water and now has to pay up to N500 daily for it to be delivered to her home
There are also the costs of giving birth in Abuja that Aliyu didn’t have back home.
To immunize her babies at the camp, the mother of nine has to take them to the nearest government hospital where nurses have certain expectations that fall to the mother, she tells FN. These include making sure the baby is wearing diapers and bringing various items including cotton wool and baby lotion, which would cost money Aliyu says she doesn’t have.
“In Borno, it was not compulsory to use [diapers] when going to the hospital. We just used our wrappers (a piece of fabric women tied around their waist). But here, the nurses insist that (the babies) must wear diapers and (we must) have an extra one in our bag,” Aliyu says. Multiple mothers shared similar concerns with FN.
Dr Charles Nzelu, Head of Special Duties at Nigeria’s Federal Ministry of Health tells FN he believes health workers are simply acting in the overall interests of the baby and that a lack of medical skill, experience, and communication is resulting in a lack of understanding about the women living in the IDP camps. “When you come to me as a doctor, I will give you medical advice the way it’s supposed to be,” he explains. “When you are more experienced, you are flexible (with) the way you relate with patients.” He adds that this government, which came into power in May, will work to address issues like these.
“I can’t afford treatment. If it happens, I’m dead”Pregnant resident of Durumi Camp in Abuja, Aisha Aliyu
In the meantime, Aliyu says she is struggling to meet all her needs and those of her children. To afford what she can, Aliyu makes and sells wigs and traditional caps worn by men, earning on average ₦10,000 ($12.49) a month.
Money is not her only concern. Aliyu worries about catching malaria and about not being able to produce enough breastmilk because of the poor quality of her diet. Her family survives on staples such as pasta and maize in different forms.
“I can’t afford the treatment” for malaria, says Aliyu. “If it happens, I am dead.”
Difficulty fulfilling promises
The National Commission for Refugees, Migrants and Internally Displaced Persons (NCFRMI) is responsible for Nigeria’s growing number of displaced people. Its commissioner tells FN that the organization, which was set up in 1989 and has a health budget of N250 million for 2024, has paid for midwives to visit IDP camps to assist in deliveries of babies as frequently as funds allow and has, in some instances, also paid off people’s hospital bills. FN was unable to verify this budget figure provided by the Commission which it said is not yet public.
However, some of the IDPs who have been in Durumi since the informal settlement formed in 2014, say that no midwives sent by the Commission have visited the camp during their time here and that in the past, it has been difficult to get it to fulfill promises they say the Commission made to the camp, such as furnishing the health post with an additional bed, scanning machine, gloves and other health equipment.
FN asked the NCFRMI about the services it provides to those in Durumi but did not receive a response prior to publication.
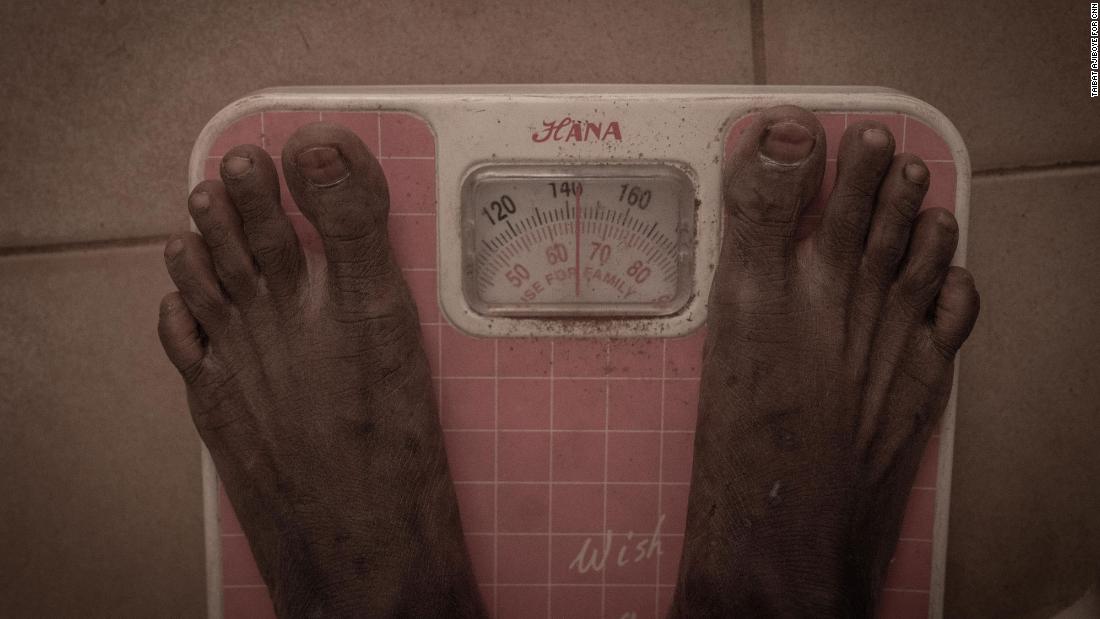
The nurse takes the weight of the pregnant women during antenatal
Within the Federal Capital Territory (FCT), where Abuja is located, the Territory’s Health and Environmental Services is responsible for all health matters including services provided to people in IDP camps, including reproductive care and sexual health services, such as birth control. Dr. Dolapo Fasawe, Mandate Secretary of the FCT Health and Environmental Services, tells FN that IDP camps in the area have functional clinics supported by area council staff and partners from outside, explaining that they cannot build permanent structures because the camps are meant to be temporary. She adds her belief that “the issue with maternal care in such places is child spacing, not maternal mortality.” Birth spacing helps to improve maternal health outcomes as becoming pregnant too soon after giving birth increases the risk of complications. Doctors FN spoke to also highlighted this as a concern in the camps, and Nigeria more widely.
But many residents of the camp told FN they had not heard of the FCT Health Services or seen them at the camp and explain that the provision of birth control is again handled by non-profits working in the camps. When Fasawe was informed of this by FN, she said it was a wakeup call for her department to act promptly. This “has opened our eyes to the need to focus on them,” Fasawe says. “We need to (conduct some) outreach asap.”
Nigeria’s Federal Ministry of Health oversees health for the country (including provisions provided by the Commission). In response to the concerns, the Ministry of Health’s Nzelu tells FN that maternal and child health is a very high priority for government but explains that the Ministry primarily provides policies and guidelines for states, local governments and government agencies to follow and does not typically intervene directly. He said: “As a government, we are still working to make sure that both the state and all these agencies of government that are charged with the direct implementation, do their best to make sure that those inhabitants of IDP camps are well taken care of.”
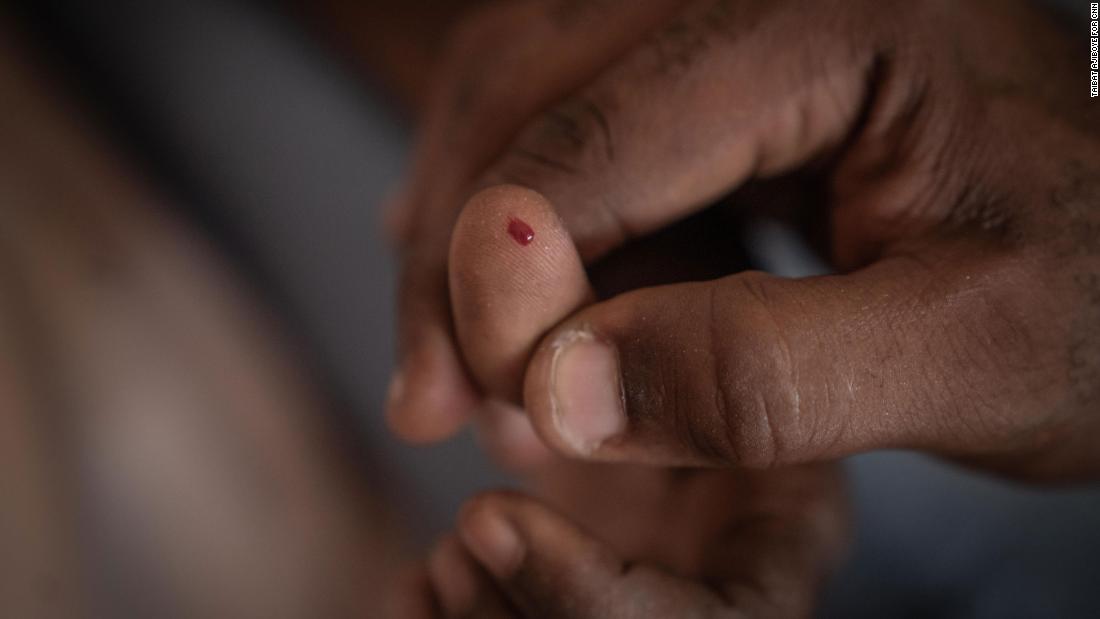
A volunteer doctor brought his own kit to do blood tests at the Durumi camp
‘A woman who falls through the cracks is falling with her children’
African NGO, Pro Health International, has been sending volunteer medical professionals to provide free healthcare services for IDPs across Nigeria for over 12 years. They were last in Durumi in June and describe it as one of the most impoverished IDP camps within the Federal Capital Territory (FCT), where Abuja is located.
Pro Health International Founder and Executive Director Dr. Iko Ibanga shared that his team raised the issue of health challenges within IDP camps two years ago with the Minister of Health at the time, Dr. Osagie Ehanire. “We were told it would be looked into, but nothing was done,” he says.
Ehanire did not directly respond to FN about whether Pro Health International raised the issue of health challenges among internally displaced people with him, but the former health minister highlighted the NGO’s work as a useful implementer of maternal health services in more recent years, and shared emergency response plans for IDPs that were put in place in the north-east of the country (where Boko Haram is most active) and go back to 2016. He tells FN: “Women’s Health services were prioritized and featured strongly in the programs designed to the needs of internally displaced women.” This region does not include Abuja, however, where the Durumi camp is located.

Women at the Durumi IDP camp, sitting on the veranda of the makeshift health post
The 2023 health budget is ₦1.17 trillion ($2.2bn), which is a 42.6% increase since 2022 and the highest percent of the total budget allocated for health. But In Africa’s largest economy, this is only 5.7% of the annual budget of ₦20.5 trillion, and is much lower than the 15% of annual budgets all African Union member nations, including Nigeria, pledged in 2001 to spend on “improvement of the health sector”.
According to the National Primary Health Care Development Agency, a health post, which is the most basic health care facility, should be able to cater to a population of 500 and have 34 items always available to serve that population. Durumi’s health post serves more than 3000 people and has just 10 of these items: a waste bin, scissors, fetoscope, weighing scale, chair, tables, two beds, kidney dishes, and a cupboard, all provided by NGOs according to Ayuba and Umar who say they both manage the facility without a salary.
Nzelu shares that the Ministry of Health is currently conducting a health needs assessment in most of the IDP camps to learn what is and is not lacking to ensure adequate health care services. He tells FN: “With the budget cycle currently on, it can inform some of the things we are able to get into the budget and hope that the National Assembly gives approval so that we can implement.”
Pro-Health International’s Ibanga is emphatic about the risks displaced people face during the perinatal period and beyond. “When [a woman] is ill, it affects everything tied to her and her children are the most important things tied to her,” he says. “A woman who falls through the cracks is not falling by herself. She is falling with her children.”




























